Oregon’s health care system will begin 2023 with a fresh start as a new director for the Oregon Health Authority takes the helm and Gov.-elect Tina Kotek is sworn into office.
James Schroeder, currently the CEO of the state’s largest Medicaid insurer, Health Share of Oregon, will serve as interim director starting Jan. 10, the same day Kotek takes office and Gov. Kate Brown’s term ends. He’ll have plenty to tackle as he takes over for Patrick Allen, who was appointed by Brown, also initially on an interim basis.
Oregon faces lingering health care issues as the pandemic wanes. They include a mental health crisis, a shortage of hospital beds that is exacerbated during surges in COVID-19, influenza or other illnesses like RSV.
There’s also an ongoing workforce shortage in health care that impacts hospitals, access to behavioral health care and other services. Other issues linked to health care and access continue to plague the state, such as homelessness and a lack of affordable housing.
Schroeder has a diverse range of experiences, from the front lines of clinics for low-income Oregonians to executive roles in large health care corporations. He has led the 426,000-member Health Share Medicaid insurer and worked in top roles at Kaiser Permanente, including vice president of safety net transformation and medical director of Medicaid. He’s also experienced as a clinician and executive in medical clinics that serve Medicaid patients and had a role in founding and leading the Neighborhood Health Center in the Portland area.

In his new role, he’ll lead an agency that spends more than $17 billion a year and has 4,770 employees. The authority’s Medicaid program, which provides health care to low-income people, covers 1.4 million Oregonians, or one in three residents.
Here’s a look at the top health care issues Oregonians faced in 2022 and what’s ahead:
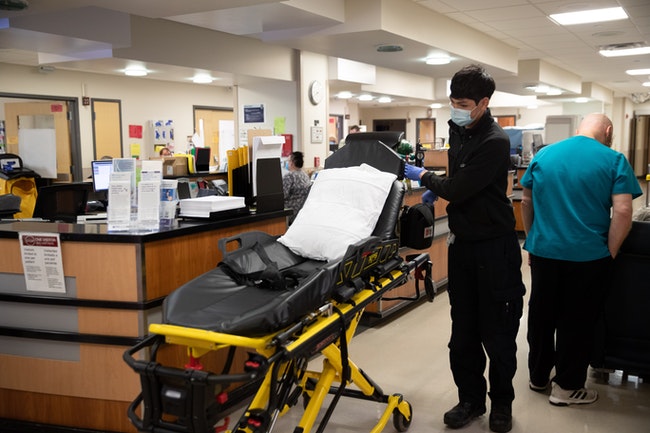
Hospitals: The pandemic exacerbated an existing shortage of nurses and other health care workers as professionals retired early or left for other work, leaving hospitals scrambling to cover openings.
Now, the workforce crisis continues even though fewer COVID-19 patients need to be hospitalized. Patients are forced to wait longer in emergency rooms for open hospital beds and hospitals have postponed some procedures.
The nursing shortages have affected patient care, they told the Capital Chronicle. Sometimes the consequences are dire, with patients dying because of a lack of staff, Patrick Allen, Oregon Health Authority director, told a legislative committee in September.
With the triple whammy of the winter season of COVID-19, influenza and RSV, or respiratory syncytial virus, the strain on hospitals affects people of all ages. They range from toddlers most susceptible to RSV to seniors and immunocompromised individuals who face the most risk from COVID-19 and influenza.
In the short-term, hospitals have turned to crisis standards of care, which allow the flexibility in assigning duties and devising schedules and give them the ability to triage care if resources run short. The Oregon Health Authority, through a staffing contractor, has hired dozens of contract nurses to shore up pediatric units in hospitals during the trifecta of illnesses.
But those are not permanent solutions. Lawmakers in the next session will hear proposals aimed at bolstering the workforce.
For example, the 15,000-member Oregon Nurses Association is backing legislation that would have a stronger enforcement mechanism and steep daily fines of up to $10,000 for hospitals that don’t abide by minimum staffing levels. Existing state law requires hospitals to develop staffing plans, but the nurses union has said more accountability is needed.
Mental health: Oregon’s mental health system continues to struggle to meet demands. The Oregon State Hospital, the state-run mental health hospital, faces tighter deadlines under a court order to admit and care for patients who need treatment to face criminal charges. Those accused of misdemeanors can stay at the hospital a maximum of 90 days; those accused of nonviolent felonies have up to six months and patients accused of violent felonies can be treated for a year.
The new deadlines came after a lengthy court battle because the state was unable to comply with a prior 2002 court order to admit patients within seven days of a judge determining they need treatment to aid in their defense.
To respond to the new deadlines, Oregon State Hospital is asking lawmakers for $4.9 million for 59 new staff positions for the rest of the biennium, which ends June 30, 2022.
But the state hospital isn’t the only part of the mental health system that is squeezed. County officials and prosecutors warn the new deadlines strain limited county community mental health services when those patients are returned to their communities and still need care.

State officials acknowledge there is a shortage of beds for residential mental health programs – another issue that lawmakers plan to address in the next session.
State lawmakers approved $1 billion in new funding during the 2021 session for various behavioral health programs. The state has dispersed or committed most of that funding, and it will take time to see the benefits.
Addiction: Moving forward, Oregon’s treatment of people with addictions will begin a new era in 2023. The state is funding Measure 110 services with about $300 million in marijuana tax revenue through June 2023. Voters in 2020 approved Measure 110, which decriminalizes low-level drug possession, with an eye toward treating addiction.
For Oregon, the state’s addiction rate stands out nationally. National reports, including this one from Mental Health America, consistently rank Oregon as having either the highest or one of the highest rates of people with mental health and addiction problems.
Critics have blasted the health authority, which oversees the program, for its slow rollout of money authorized by the measure. It was finally distributed by this summer, about a year later than scheduled. At the same time, the agency approved mental and addiction networks in each of Oregon’s 36 counties. They offer a range of services, including health screenings, addiction treatment and assistance so people can find housing and employment.
But it will take months before they will have an impact. Kotek has said she wants the system to continue but has said she will keep a close eye on developments.
Oregon Capital Chronicle is part of States Newsroom, a network of news bureaus supported by grants and a coalition of donors as a 501c(3) public charity. Oregon Capital Chronicle maintains editorial independence. Contact Editor Lynne Terry for questions: [email protected]. Follow Oregon Capital Chronicle on Facebook and Twitter.
STORY TIP OR IDEA? Send an email to Salem Reporter’s news team: [email protected].

Ben Botkin - Oregon Capital Chronicle
Ben Botkin covers justice, health and social services issues for the Oregon Capital Chronicle. He has been a reporter since 2003, when he drove from his Midwest locale to Idaho for his first journalism job. He has written extensively about politics and state agencies in Idaho, Nevada and Oregon. Most recently, he covered health care and the Oregon Legislature for The Lund Report. Botkin has won multiple journalism awards for his investigative and enterprise reporting, including on education, state budgets and criminal justice.